Latest blog posts
Get expert advice from our library of articles. Whether you’re curious about your skincare journey, or the ins and outs of actives, our posts are full of dermatologist-approved tips to help you achieve the #DermaticaDifference.
February 19, 2024
0 Comments7 Minutes
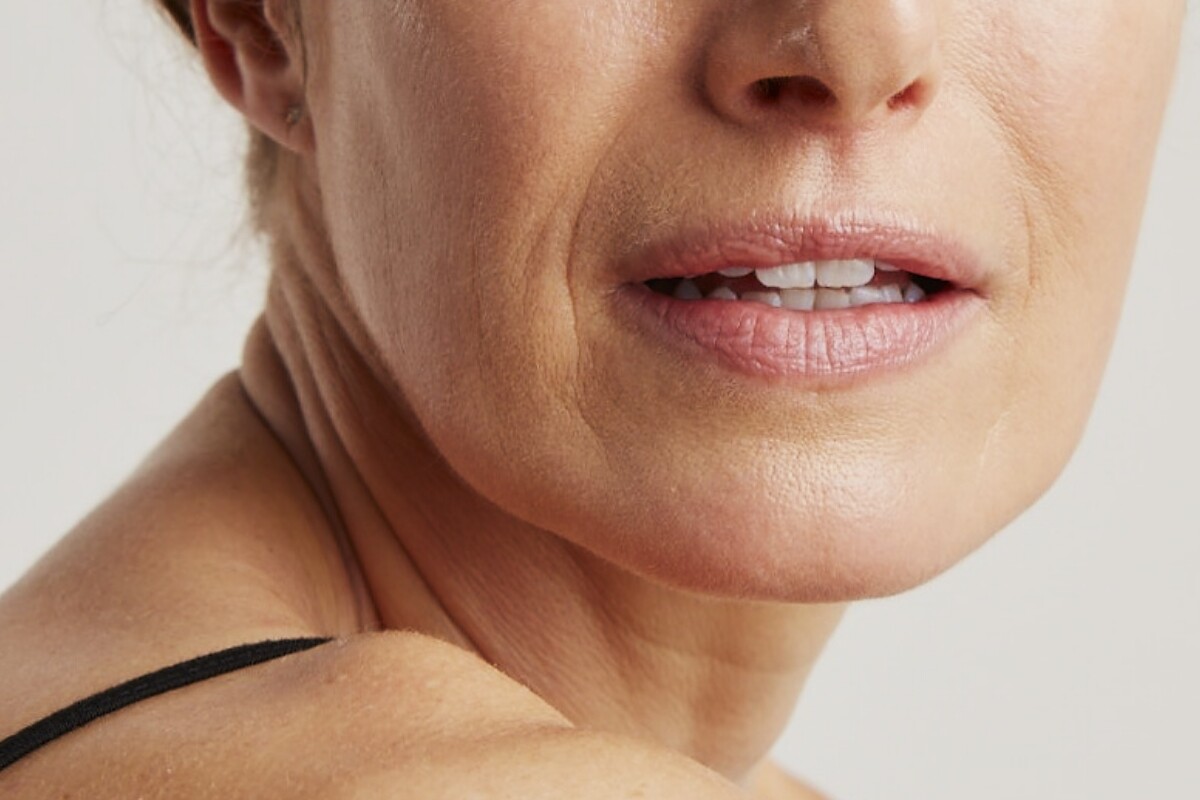
Retinoids, Vitamin C and sunscreen: the evidence-based trio for younger looking skin
February 19, 2024
0 Comments14 Minutes
Under the Microscope: When Will I See Results from Tretinoin and Retinoids?
January 15, 2024
0 Comments5 Minutes
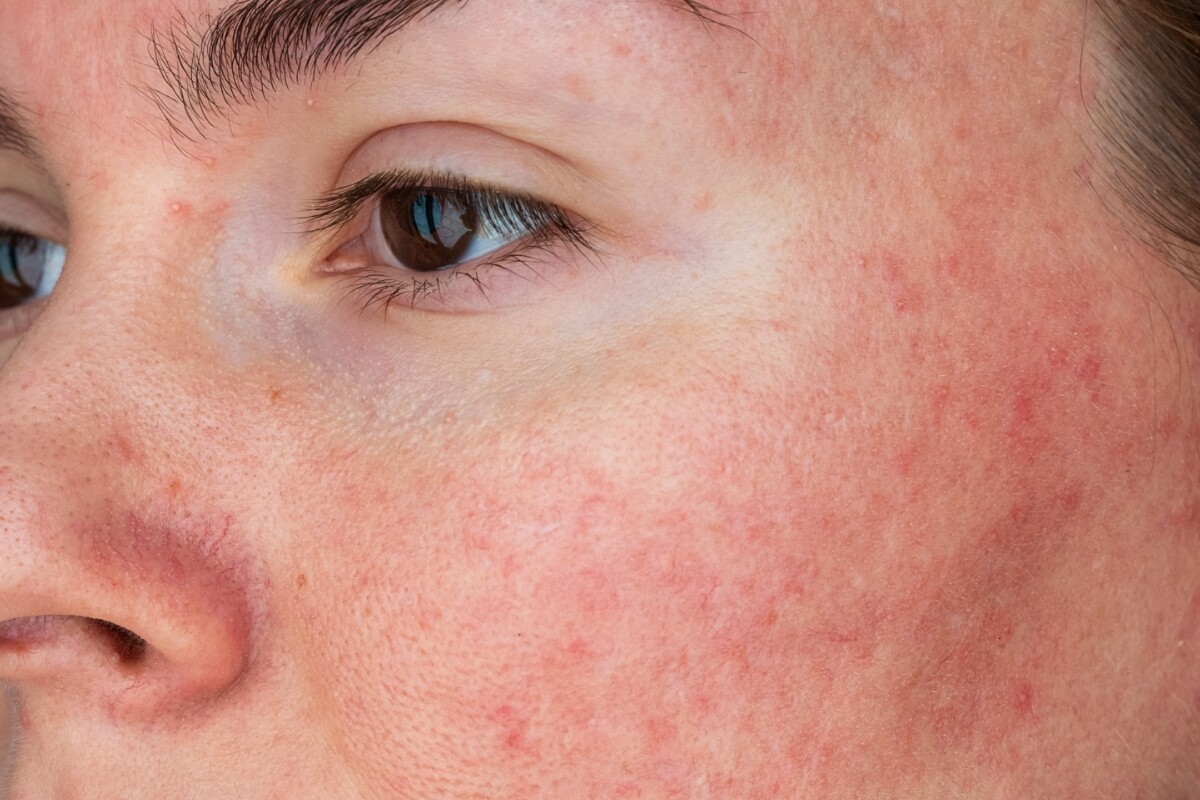
Under the microscope: Oral Antibiotics for Acne, Rosacea and Pigmentation
January 8, 2024
0 Comments6 Minutes
Why everyone’s talking about tranexamic acid for hyperpigmentation